Australia's Generic Market: PBS Overview and Impact
December 8 2025Cervical Ripening: What It Is and How to Prepare
If your doctor has talked about inducing labor, they probably mentioned cervical ripening first. A soft, thin cervix is the gateway for a baby to move down, so before contractions start we need the cervix to open up a bit. That’s what cervical ripening does – it gets the cervix ready, making induction safer and more effective.
How Cervical Ripening Works
The cervix stays firm for most of pregnancy because hormones keep it closed. As you near term, the body releases prostaglandins and relaxin, which soften the tissue and thin it out (called “effacement”). When we speed up this natural shift with medication or a device, we call it cervical ripening.
Doctors often check two scores before starting: the Bishop score. It looks at dilation, effacement, position, consistency, and how far down the baby’s head is. A low score means the cervix needs more work; a higher score suggests you’re already close to going into labor on your own.
Choosing the Right Method
There are two main families of ripening tools – drugs and mechanical devices. Each has its own vibe, so talk with your provider about what fits your situation.
Prostaglandin gels or tablets: These are applied to the cervix or placed in the vagina. Common brands contain misoprostol or dinoprostone. They mimic the body’s natural prostaglandins and usually start softening the cervix within a few hours. You might feel mild cramping, spotting, or a low‑grade fever – all normal signs that it’s working.
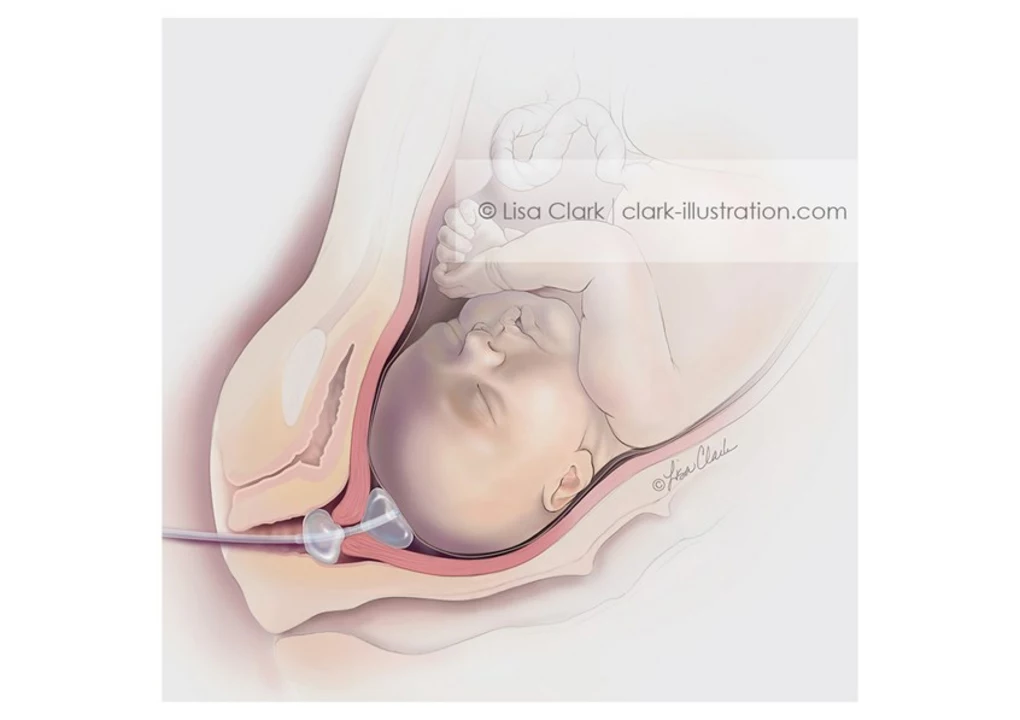
Insertable balloons (Foley catheter): A small tube with a balloon is slipped through the cervix and inflated. The pressure gently pushes the cervix open while also stimulating prostaglandin release. Many women find this method less likely to cause intense uterine contractions before they’re ready.
Combination approaches: Some clinics start you on a low‑dose prostaglandin, then add a Foley if progress stalls. This can speed things up while keeping side effects in check.
When deciding, consider your health history. If you have a scarred uterus or previous C‑section, doctors might avoid strong prostaglandins because they could trigger too‑quick contractions. Mechanical methods are often safer in those cases.
What to expect during ripening: You’ll likely stay at the hospital or a birthing center for monitoring. Nurses will check your cervix every few hours and watch for signs of active labor, like regular painful contractions. If you feel strong cramping early on, let the staff know – they might adjust the dose or remove an insert.
Side effects are usually mild: nausea, low‑grade fever, or watery discharge. Rarely, the cervix can over‑ripen and start strong contractions too soon; that’s why continuous monitoring is key.
After ripening is done, you move straight into induction with oxytocin (Pitocin) or continue waiting for natural labor if the cervix has opened enough.
Tips to make it smoother:
- Stay hydrated – fluids help your body respond to medication.
- Move around if allowed; gentle walking can encourage cervical change.
- Ask about pain relief options before the process starts, so you’re not surprised.
- Keep a list of questions handy: How long will ripening take? When will I be moved to labor?
Remember, cervical ripening is just one step on the road to meeting your baby. It’s designed to give you and your provider more control over timing while keeping both of you safe. If something feels off, speak up – the team is there to adjust the plan for your comfort.
 9 May
9 May
The Benefits of Misoprostol in Cervical Ripening and Labor Induction
As a blogger, I've recently been exploring the benefits of Misoprostol in the process of cervical ripening and labor induction. I've discovered that Misoprostol is an effective and affordable option for many women, especially in low-resource settings. It helps to soften and prepare the cervix for labor, resulting in a smoother and safer delivery process. Additionally, it can be administered orally or vaginally, providing flexibility for both healthcare providers and patients. In conclusion, Misoprostol is a valuable tool in promoting positive childbirth experiences and reducing complications.
Read More...