Managing your INR while on warfarin isn’t just about taking your pill on time. It’s about what’s on your plate. A single cup of kale can drop your INR from 2.8 to 1.9 in days. A switch from spinach to iceberg lettuce might spike it to 4.1. These aren’t rare cases - they’re everyday stories from people living with blood thinners. The truth? vitamin K isn’t your enemy. It’s your balancing act.
How Warfarin and Vitamin K Work Together
Warfarin doesn’t thin your blood. It slows down how fast your blood clots. It does this by blocking vitamin K from doing its job. Vitamin K is what your liver uses to build clotting factors - proteins that stop you from bleeding out after an injury. Without enough vitamin K, those proteins don’t form properly. Warfarin steps in and makes sure there’s not enough active vitamin K around. That’s why your blood takes longer to clot.
But here’s the catch: vitamin K from food doesn’t disappear after one meal. It builds up in your liver. If you eat a lot of vitamin K one day and almost none the next, your body’s clotting system gets confused. One day, warfarin is working fine. The next, your vitamin K intake overwhelms it. Your INR drops. You’re at risk for clots. That’s why consistency matters more than avoidance.
Which Foods Have the Most Vitamin K?
Not all vegetables are created equal when you’re on warfarin. The American Heart Association uses a clear cutoff: foods with more than 60 mcg of vitamin K per serving are considered high-risk. Here’s what that looks like in real portions:
- 1 cup cooked kale: 547 mcg
- 1 cup cooked spinach: 889 mcg
- 1 cup cooked broccoli: 220 mcg
- 1 cup raw parsley: 246 mcg
- 1 cup cooked Brussels sprouts: 219 mcg
- 1 cup raw lettuce (iceberg): 17 mcg
- 1 cup cooked cabbage: 109 mcg
- 1 cup cooked green beans: 28 mcg
These numbers aren’t guesses. They come from the Academy of Nutrition and Dietetics’ 2018 food database, updated with lab-tested values. A single cup of kale has more vitamin K than the entire daily recommended intake for a healthy adult (90-120 mcg). That’s why people who suddenly add kale smoothies to their routine often end up in the ER.
Why Consistency Beats Restriction
For years, doctors told patients on warfarin to avoid vitamin K-rich foods. That advice has changed. The 2023 American College of Chest Physicians Guidelines now say: don’t cut out vitamin K. Just keep it steady.
Here’s why: if you eat 500 mcg of vitamin K every day, your body adapts. Warfarin can be adjusted to match. But if you eat 500 mcg one day and 50 mcg the next? Your INR swings like a pendulum. Studies show that patients who kept their daily vitamin K intake within 10% variation had a 70%+ time in therapeutic range (TTR). Those with inconsistent intake? Only 34% stayed in range.
One patient in a 2019 study ate exactly 1 cup of cooked broccoli (220 mcg) every single day for six months. His TTR hit 92%. He didn’t avoid broccoli. He just made it part of his routine.
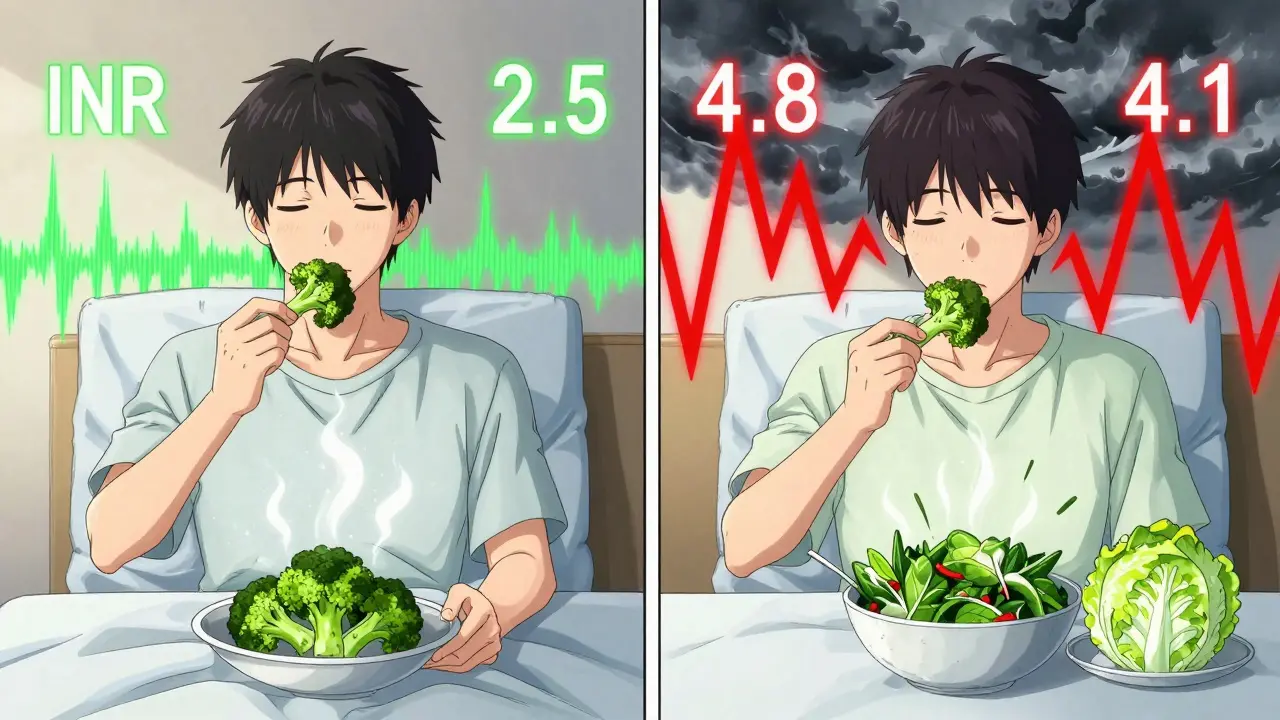
What About Cooking and Prep?
How you cook your greens changes vitamin K content. Boiling spinach or kale for 10 minutes can knock out 30-50% of the vitamin K. Steaming? It preserves almost all of it. Raw salads? Higher vitamin K than cooked. That’s why a raw spinach salad (145 mcg per cup) is safer than a boiled one (889 mcg per cup).
Also, don’t assume all brands are the same. Frozen spinach is often blanched before freezing, which reduces vitamin K. Fresh, uncooked spinach? High. A salad with fresh kale and raw broccoli is a different beast than a steamed side of the same veggies.
What About Other Sources of Vitamin K?
Most people think vitamin K only comes from leafy greens. It doesn’t. Vitamin K2 (menaquinone) is found in animal products and fermented foods:
- Natto (fermented soy): 1,103 mcg per 100g - extremely high
- Goose liver: 100 mcg per 100g
- Hard cheeses (cheddar, gouda): 50-75 mcg per 100g
- Egg yolk: 10-20 mcg per yolk
- Chicken liver: 70 mcg per 100g
Natto is a big one. It’s common in Japanese diets and contains more vitamin K2 than any other food. If you eat natto regularly, your warfarin dose will need to be higher. If you stop eating it suddenly? Your INR could rise dangerously.
Supplements are another hidden risk. Many multivitamins contain vitamin K. Some probiotics boost vitamin K2 production in your gut. Even certain herbal teas (like nettle or alfalfa) have vitamin K. Always check labels. A daily 100 mcg supplement might seem harmless - until it throws off your INR.
How to Stay on Track
You don’t need to become a nutritionist. But you do need a simple system:
- Choose 1-2 consistent sources of vitamin K. Pick one high-vitamin K food (like broccoli or kale) and eat the same portion every day. If you like spinach, stick to one type - don’t switch between raw, cooked, frozen, and fresh.
- Use a food tracker. Apps like CoumaDiet (rated 4.6/5 by over 1,200 users) log vitamin K content automatically. Take a photo of your meal, and it tells you the estimated intake.
- Plan your meals weekly. If you’re having kale on Monday, have it on Tuesday too. No surprises.
- When dining out, ask how food is prepared. Steamed? Raw? Sautéed? The difference can be 200 mcg of vitamin K.
- Keep a log of your INR readings alongside your meals. Look for patterns. Did your INR drop after eating a big salad? That’s your clue.
Patients who followed these steps for 6 weeks saw a 37% drop in INR instability, according to the Canadian Journal of Cardiology. That’s not magic. That’s structure.
When Things Go Wrong
Even with the best intentions, mistakes happen. You eat a big plate of kale at a friend’s house. Your INR crashes. What now?
Don’t panic. Don’t skip your next warfarin dose. Don’t try to “fix it” with a vitamin K pill. Talk to your anticoagulation clinic. They might:
- Temporarily increase your warfarin dose
- Give you a low-dose oral vitamin K pill (100-200 mcg) to stabilize your INR
- Reschedule your next INR test to 2-3 days later
A 2018 study in the Journal of Thrombosis and Haemostasis found that 83% of patients with high INR returned to normal within 7 days after taking 100-200 mcg of vitamin K. It’s not a cure. It’s a tool.
On the flip side, if your INR spikes (above 4.0), you might need to reduce warfarin or temporarily stop it. But never do this without medical guidance. A high INR means bleeding risk. A low INR means clot risk.
What About DOACs? Are They Better?
Direct oral anticoagulants (DOACs) like apixaban and rivaroxaban don’t interact with vitamin K. That’s why they’re popular. But they’re not for everyone. If you have a mechanical heart valve, you’re still on warfarin - 98% of those patients are. Same goes for antiphospholipid syndrome. DOACs don’t work as well there.
Even with DOACs, vitamin K matters. It’s not about blood clotting. It’s about bone health and artery calcification. But for INR control? Only warfarin users need to track it.
Final Takeaway
You don’t need to eat bland, vitamin K-free meals. You need to eat the same meals, consistently. One cup of broccoli every day. One serving of kale twice a week. No sudden changes. No wild swings between spinach and lettuce. Your INR will thank you.
Stable INR means fewer hospital visits. Fewer dose changes. Less anxiety. It’s not about perfection. It’s about predictability. Your body doesn’t like surprises. Neither does warfarin.
Can I eat leafy greens while on warfarin?
Yes - but only if you eat the same amount every day. A cup of cooked spinach every day is fine. Eating spinach one day and iceberg lettuce the next will throw off your INR. Consistency matters more than avoidance.
What happens if I eat too much vitamin K one day?
Your INR will likely drop, meaning your blood clots faster. This increases your risk of stroke or clotting. Don’t skip your warfarin. Contact your clinic. They may adjust your dose or give you a small amount of vitamin K to help stabilize your levels.
Should I take a vitamin K supplement?
Only if your doctor recommends it. For people with erratic diets, a daily 150 mcg vitamin K supplement can actually stabilize INR. But for most, it’s unnecessary and risky. Never take supplements without talking to your anticoagulation team.
Does cooking reduce vitamin K in vegetables?
Yes - boiling can reduce vitamin K by 30-50%. Steaming, sautéing, or eating raw preserves more. That’s why a raw kale salad has more vitamin K than steamed kale. Track how you prepare your food, not just what you eat.
How often should I get my INR checked?
Monthly is standard, but if your diet changes or you’re new to warfarin, you may need checks every 1-2 weeks. Once your diet and dose are stable, you can go to every 4-6 weeks. Always follow your clinic’s schedule - don’t skip tests.
Can I drink alcohol while on warfarin?
Moderate alcohol (1 drink per day for women, 2 for men) is usually fine. But binge drinking or heavy daily use can increase bleeding risk and interfere with how your liver processes warfarin. Consistency matters here too - don’t switch from no alcohol to 3 drinks on weekends.
What if I’m traveling or eating out?
Plan ahead. Use apps to estimate vitamin K content. Ask restaurants how food is prepared. Stick to familiar dishes. Avoid large salads, kale, spinach, or fermented foods like natto. Bring a small food log to track what you eat. Many patients have emergency INR changes after travel - planning prevents it.
Staying on warfarin isn’t about fear. It’s about rhythm. Find your routine. Stick to it. Your body will keep you safe.